Vital signs:
BP: 82/40
P: 49
R: 16
Sp02: 86% on room air
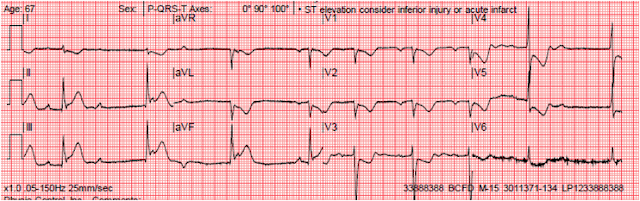
12 Lead ECG Discussion
The rhythm is sinus bradycardia. Unless this 80 year old is a marathon runner, the rate is abnormal. Furthermore, the bradycardia occurs in association with (1) near syncope and (2) abnormal vital signs. ST segment elevation is seen in leads II, III, and aVF. Reciprocal change in the form of ST segment depression is seen in lead aVL. STE is also observed in the lateral precordial leads. The R waves are tall in V2 and V3 but there is no concurrent ST segment depression to suggest involvement of the heart's posterior wall. Q waves, though not pathologic, appear in leads II, III, and aVF, and favor the diagnosis of ischemia.
12 Lead ECG Interpretation
Sinus bradycardia, Inferior-lateral ST segment myocardial infarction.
Case Discussion
This case presents more than a few dilemmas and teaching points. First, it emphasizes the association between dizziness, weakness, and acute coronary syndromes. Elderly patients may not present with the classic "chest pain" or "chest pressure." Dyspnea, dizziness, and weakness are well known anginal equivalents and should be aggressively investigated, especially in the setting of abnormal vital signs. The presence of peaked T waves might suggest underlying hyperkalemia. The changes associated with hyperkalemia are usually diffuse. The STE in this ECG follows an anatomic (inferior-lateral) pattern. If there is concern for "abormal labs," then the administration of calcium is probably warranted. Calcium should always be considered first line in the management of hyperkalemic emergencies.
What About the Rate?
This patient also presents with symptomatic bradycardia. A well accepted axiom in EMS and emergency medicine is, "fix the rate FIRST." EMS protocols would probably advocate for a healthy dose of atropine. Ischemia of the SA node (caused by RCA occlusion) can certainly result in a symptomatic bradycardia, heart blocks, and other types of badness. However, be cautious when administering atropine to a patient suffering from an active MI. Atropine will increase myocardial demand and have the potential to exacerbate ischemic symptoms. A gentle fluid bolus may suffice to mitigate hypotension, and opening of an occluded RCA will make everything right as rain...
KEY POINTS:
- Fix the rate first (WITH CAUTION in cases of active ischemia!)
- Calcium is first line in the treatment of suspected hyperkalemia and ECG changes
- Weakness, dizziness, and syncope should be regarded as anginal equivalents- especially in the elderly
- Inferior wall myocardial infarction can produce bradycardia, heart blocks, and syncope
Special thanks to JoElyn for providing these ridiculously complex ECGs! (And best wishes as a newly minted registry medic...)